by Nutrilicious | Jul 24, 2025 | Retail, Hot Topics in nutrition, Thoughts, The Nation’s Health, Catering/Out of Home, Communications, Impactful health initiatives
At Nutrilicious, we believe that good nutrition should be accessible to everyone – especially during times of increased financial pressure. The summer holidays, while full of potential for family connection and rest, can be an incredibly stressful period for many households across the UK, particularly when it comes to putting food on the table.
For families already navigating tight budgets, the absence of free school meals and the need for more at-home meals and snacks significantly heightens food costs – and with it, food insecurity.
That’s why we’re proud to support the relaunch of the Iceland Food Club, a vital initiative from Iceland Foods in partnership with not-for-profit lender Fair for You, which provides interest-free loans of up to £75 to help families manage food spending over the summer break.
As part of our commitment to improving the nation’s nutrition, our sister company, MyNutriWeb, contributed nutrition expertise to this project – ensuring the solution is not only affordable but also nutritionally sound.
The Need Is Clear – and Urgent.
Recent research by Iceland Foods reveals the scale of the issue:
- 85% of parents report increased food bills over the summer
- This equates to a £553 million weekly increase in food spending across UK households
- The rise is driven by the need for more at-home food (73%) and the cost of extra snacks and drinks (68%)
With this in mind, the Iceland Food Club aims to provide practical and immediate relief.
What Is the Iceland Food Club?
Eligible families can access an interest-free loan of up to £75 loaded onto a pre-paid card for use in Iceland stores or The Food Warehouse. Repayable in £10 weekly installments, this initiative enables families to manage food costs without turning to high-interest options or sacrificing essentials.
Importantly, returning customers who’ve repaid their loan can top up to £100 during school holidays, helping ensure consistent access to nutritious meals.
“The summer holidays should be a time for families to relax and make memories, not worry about how they’re going to afford their next food shop… When we hear that nearly a quarter of parents are skipping meals so their children can eat, we know we have to step in.”
— Richard Walker, Executive Chairman, Iceland Foods
“The summer break is always one of the most financially stressful times of the year. With the rising cost of living, we’re expecting this to be our busiest period to date.”
— Simon Dukes, CEO, Fair for You
Our Role: Supporting Nutrition on a Budget
At Nutrilicious, we know that affordability should never mean compromising on nutrition. That’s why our expert dietetic team at MyNutriWeb proudly supported the creation of a budget-friendly shopping basket. Designed to stretch the £75 loan for maximum nutritional value, the shopping basket aligns with the UK Eatwell Guide and supports healthy, balanced meals.
This evidence-based basket is tailored for a family of two adults and two children under five, offering:
- 126 balanced portions including 5 breakfasts, 4 lunches, 5 dinners, and 7 snacks
- Recipes that are easy to prepare, affordable, and child-friendly (like banana pancakes, chilli sin carne, and chickpea wraps)
This is more than a collection of meals – it’s a tool for empowering families to shop and cook with confidence, even under financial stress.
“Working with Iceland Food Club to create this Eat Well-aligned basket is so important – it gives parents the means and confidence to buy fresh fruit, vegetables, and essentials available in Iceland supermarkets.”
— Tanya Haffner, CEO and Founder, MyNutriWeb
Why This Matters to Nutrilicious
We’re proud to be part of this initiative because it reflects everything Nutrilicious stands for – practical, impactful solutions that bridge the gap between food insecurity and good nutrition. The impact of food insecurity goes far beyond hunger; it affects mental health, children’s development, and family wellbeing.
How You Can Help
As part of our wider community of health professionals, communicators, and organisations, we encourage you to:
Small steps like sharing this initiative can make a real difference for families this summer.

by Nutrilicious | Jul 18, 2024 | Thoughts, Impactful health initiatives, Resources worth having
Informed employees empowered with the latest research and thinking in nutrition and health are the greatest asset of any food- or health-based organisation. Ensuring your teams have regular opportunities to expand and deepen their knowledge is critical to safe, effective and compliant practice. And of course it clearly demonstrates an employer’s commitment to its workforce.
Short-form courses for employees
Our sector is fortunate in having a wide range of learning resources, ranging from one-off webinars to longer-form training, but it isn’t always easy to identify which your organisation and employees will benefit most from.
For the last year Nutrilicious has been proud to partner MyNutriCourses – a programme of short, online courses designed to provide professional development learning opportunities at individuals’ own pace, in current, relevant topics.
Developed by MyNutriWeb, the team behind award-winning CPD webinars, the courses are designed to provide deeper engagement with key topics with clear practical applications.
The courses are based on the same evidence-based and high-quality research approach that feature in the webinars, but material is more expansive, with quizzes and self-reflection built in.
Presenters are highly experienced professionals including nutritionists, dietitians, psychologists, academics and other world-class experts on specific subject areas.
The short course format means that significant development of understanding is possible within the duration of one or two days, with the pace of study set however the participant chooses over 12 months. It can be fitted in within working hours or outside. And a certificate at the end of the course, accredited by relevant industry bodies, provides confirmation of achievement for CPD purposes.
Two courses have been released so far: Recipe Analysis and Sustainable Diets and Nutrition.
Practical skills in recipe analysis
The Recipe Analysis course [Recipe Analysis 101], endorsed by the Association for Nutrition, helps professionals to develop confidence, knowledge and skills in the analysis of recipes, and learn how to utilise and effectively communicate nutritional, health as well as environmental benefits through clear labelling and marketing. It’s designed for those new to recipe analysis or those wanting to refresh on the latest knowledge and skills.
There are many uses for recipe analysis, including in nutrition and dietetics, food technology, public health policy, research, marketing and more.
Having the correct training in the subject is critical. The British Dietetic Association recommends that “recipe analysis should only be undertaken and/or supervised by experienced registered dietitians or registered nutritionists, who can appropriately interpret both the input data and the results, are aware of food regulations and the limitations of their software”.
The MyNutriCourses Recipe Analysis course helps educate on the crucial considerations and steps involved when calculating the nutritional content of recipes and environmental impact communicating the results incorporating nutrition and health claims and other legal considerations.
Nutrition and sustainability upskilling
The Sustainable Diets course [Sustainable Diets] endorsed by the Association for Nutrition and the British Dietetic Association, explores the fundamental principles of sustainable nutrition for human and planetary health.
Sustainability is a key area for organisations to upskill their employees in as they tackle the urgent challenge of climate change in their day-to-day operations. Understanding healthy sustainable diets is now an important competency for all dietitians and nutritionists and is increasingly being built into job roles and educational curricula.
Following the Environment Act 2021 and the Health and Care Act 2022, legislation has set net zero goals for the NHS, the first healthcare system to have sustainability embedded. ‘Delivering a Net Zero NHS’ [https://www.england.nhs.uk/greenernhs/publication/delivering-a-net-zero-national-health-service/] highlights the goal to be net zero by 2035, with procurement to be net zero by 2040.
Many other organisations have set their own environmental, social and governance which incorporate action on sustainable eating as appropriate, with dietitians, nutritionists and other HCPs contributing to these goals at all levels.
And the newly published Allied Health Professions (AHP) curriculum guide [Guidance education for sustainable healthcare] for environmental sustainability sets out sustainable healthcare guidance within UK pre-registration curricula for allied health professions.
There have been few easily accessible training resources on the topic available to date. The MyNutriCourses Sustainable Diets course provides a comprehensive and practical foundation in the topic.
It brings together leading experts across every aspect of sustainable diets, integrating planetary and nutrition science, together with behaviour change tactics and specific considerations such as low-income groups, athletes, children and the older population.
Make an enquiry
Group bookings for both training courses are available for organisations looking to elevate the nutrition and sustainability credentials of their employees.
You can find out more at MyNutriCourses Email hello@mynutriweb.com for details of group bookings.
If you’d like to read more from the team at Nutrilicious, visit our Blog page

by Nutrilicious | Apr 16, 2019 | The Nation’s Health, Changing mindset, Impactful health initiatives
We’re excited to be involved in a new initiative to help tackle the critical problem of poor diet amongst lower income households: Shop Well – Eat Well. It’s a collaboration between the British Dietetic Association (BDA), Alpro and the Southwark Hub, with the aim of a multi-angled approach to have a real and lasting impact.
Launched last month, we brought together experts to give their insights into key topics. Here’s a summary of some of the key points, followed by links to each of the presentations, which we highly recommend you take the time to watch!
People on lower incomes have a worse diet and shorter life expectancy
There is a direct correlation between diet and income, in turn affecting health. The lower your income, the more likely it is you will:
- Eat more sugar, processed foods, fat and sodium
- Eat less fibre, vitamin A and folate
- Be less likely to meet iron, folate and calcium recommendations
- Eat less oil-rich fish
- Eat more take-aways
- Cook less at home from scratch
People in lower income groups in the UK have a significantly shorter life expectancy than the average: by nine years for women and seven for men.
They have double the rates of cardiovascular disease, lifestyle-related cancers, type 2 diabetes and total mortality compared to the national average. Obesity prevalence of the most deprived 10% of children is approximately twice that of the least deprived 10%.
This is not new news. Countless attempts have been made to try to address the problem and encourage people on lower incomes to eat more healthily, thereby increasing their quality of life and life expectancy.
But when it comes to eating habits, behaviour change is very difficult to achieve.
Barriers to healthy eating are multiple, complex and interlinked – psychological, financial, environmental, conscious and unconscious. Among lower income households they include:
- Financial barriers – For low income families, a big barrier to buying new foods or going to a new food shop is not knowing how much the food will cost, or assuming that it will all be expensive. Parents want to know exactly how much their shopping basket is before they reach the checkout.
- Social barriers – Food habits get passed down the generations as young people grow up and become parents themselves. What children see their parents and families doing is what they grow up thinking of as ‘normal’.
- Preparation space – Cooking from scratch relies on kitchen equipment, confidence in cooking skills, time to prepare food and pleasant surroundings – not the case for many on low income.
- Limited bandwidth – The cognitive burden of living under financial strain and other modern day life stresses reduce parents‘ mental bandwidth; brainpower that would otherwise go to planning ahead and problem-solving.[1] Families in this situation look for quick and easy ways to eat, and takeaway and convenience foods provide an in-the-moment solution to feeding children quickly, affordably and safely.
- Advertising and shop layouts – Cues such as special offers, advertising for takeaways, attractive packaging and child-height shelving nudge families towards less healthy foods in shops.
- It’s not always a lack of knowledge or cost that’s a problem, it’s translating knowledge to practice.
In fact, most eating behaviour is driven by unconscious, habitual processes. These are largely immune to education when it comes to behaviour change. Yet this has been our predominant approach to changing dietary behaviour!
Breaking the habits of a lifetime
Multiple collaborative strategies are needed to succeed in changing behaviour: from government, local authority, industry and all food providers, alongside continuing to help individuals overcome their personal barriers.
We need to making healthy eating
- easy,
- habitual, and
- normal
As behavioural psychologist Dr. Paul Chadwick says, it’s not sustainable for people to have to think about every food choice that they make. Healthy eating has to become the default option.
A new initiative for change
Behavioural science shows the importance of interactions between the individual and their physical and social environment when it comes to habit forming and breaking.
It’s time the food environment changed to make healthy eating as easy to attain as possible for all, including low affluent groups.
It’s also time for families and individuals to be supported in overcoming barriers to breaking the unhealthy habits.
 We’re excited to be part of the new initiative, Shop Well – Eat Well, to help enable this – especially targeting those on a low income.
We’re excited to be part of the new initiative, Shop Well – Eat Well, to help enable this – especially targeting those on a low income.
Starting as a year-long pilot in Southwark, South London, it’s kicking off in June. Community charities and volunteers will join to create peer and professional-led healthy eating seminars and workshops tailored to the young, old and families.
At the launch, Kate Arthur, UK External Scientific Affairs & Nutrition Manager at Alpro, explained: “We wanted to find interventions that would encourage people to think about their food choices differently.
“Going directly into the community to find out what will work for people is the logical thing to do. We’ll be working on different engaging activities such peer led cookery workshops and drop in seminars, with help from the BDA Let’s get Cooking and an advisory committee of experts, always with an eye on the main barriers.
“Ultimately, we’ll be assessing to see what really makes a difference over the next year of the campaign and we’ll share any success stories widely with local communities nationwide and the dietetic community as a whole.”
Caroline Bovey, Chair of the British Dietetic Association added: “By partnering on this project, and working with the food manufacturers and shops that people are accessing daily, we’re excited to directly tackle some of the wider barriers to healthy habits in a local area. The BDA is delighted to be working with Alpro and the Southwark wellbeing hub to help people who often have to prioritise the other demands of daily life over their food choices.”
Take advantage of insightful presentations and useful resources
At our launch, five leading experts presented the latest evidence and initiatives to help overcome barriers to healthy shopping baskets and healthy eating. The presentations are available on the Shop Well – Eat Well website. Make yourself a cup of tea, watch, learn and be inspired:
– Dr Paul Chadwick, behaviour change leading expert: A scientific approach to behaviour change
– Sue Baic, Registered Dietitian: Affordable, healthy and sustainable eating in practice
– Duncan Brown, Development Director at charity Shift design: How does affluence impact on food choices?
– Kate Arthur, Alpro UK’s External Scientific Affairs & Nutrition Manager: Changing behaviour in the community
– Nilani Sritharan, Company Nutritionist at Sainsbury’s Supermarkets Ltd: Making healthy shopping easier
You’ll also find practical and engaging resources to help consumers overcome their barriers to healthy eating.
#shopwelleatwell @SouthwarkHub @BDA_Dietitians @Alpro

by Tanya HAFFNER | Nov 12, 2018 | Changing mindset, Impactful health initiatives
The facts are now mounting that our food choices not only impact our health but are also fast depleting the planet’s resources.
Taking into account every stage from production, distribution and delivery through to waste, we see the sizeable impact our food choices have on the environment. What we eat:
- Contributes 20-30% of total greenhouse gas (GHG) emissions
- Is the leading cause of deforestation, biodiversity loss and soil and water pollution
- Accounts for 70% of all human water use
- Is responsible for global inequality: current food production is adequate to meet the needs of the global population of 7 billion, however, 2 billion exceed their needs whilst 800 million suffer hunger
Additionally, 30–50% of all food produced is spoiled or wasted.
If we’re going to save our planet, we need to change the way we eat.
Choosing a sustainable diet
For the first time, the UK government’s most recent Eatwell Guide acknowledged the importance of eating to help sustain the planet, as well as for health.
It was modelled to ensure that all macro and micronutrient needs of people aged 5 and over are met, while the nation’s carbon footprint is reduced by almost one third.
- Supporting our planet
The Eatwell Guide recommends that 80% of food we consume should be of plant origin: the focus is on reducing meat – especially beef – and dairy, which have the most impact on the world’s resources.
– Livestock production is by far the most significant contributor to GHG emissions (methane, carbon dioxide and nitrous oxide) contributing to 14.5% of all GHG emissions.
– Cattle consume 40% of all grains produced. Over one third of arable land is dedicated to growing grains solely for animal feed production.
– Livestock is the main cause for deforestation, biodiversity loss, degradation and water pollution.
- Improving our health
The benefits come not only to the planet but also our health. As we discussed in our blog on the popularity of vegetarian and vegan diets, it is well established that diets higher in plant foods and lower in meat products result in a lower intake of both energy (calories) and saturated fat, while increasing fibre intake.
Those with a plant-based diet suffer significantly less from diseases such as obesity, type 2 diabetes, cancer and heart disease.
The barriers to change
With only 1% of the population adhering to the previous (and less plant-based) Eatwell plate, how can we now expect people to adopt a more environmentally-friendly diet?
The British Dietetic Association is committed to bringing sustainable diets to the top of the dietetic agenda. They’ve put together a new toolkit providing both scientific knowledge and the practical tools to empower dietitians and consumers to adopt a diet focussed on sustainability.
The advice follows extensive research into the science of sustainable eating and top barriers and motivators. These were identified as:
- Lack of practical knowledge and resources
- Perceptions that sustainable healthy eating requires more time, more money and taste has to be compromised.
- What’s on offer from retailers, restaurants, take-aways, etc. – with an imbalance toward unhealthy, plant-based foods versus health and affordable plant foods?
- Language needing to be tailored to the audience depending on culture, age group, socio-economic and education status
- Clarity over messaging, for example on fish and processed foods
- The misconception of sustainable only associated with vegetarian/vegan diets, and of them being nutritionally inadequate
Sound familiar? Have you been able to overcome the barriers and use successful motivators to increase your own sustainable eating, or that of a client?
Be first to benefit from the BDA’s Sustainable Diet toolkit
We are giving an exclusive preview of the toolkit along with an overview of the latest science on the upcoming FREE CPD NutriWebinar on Sustainable Diets, 14 November 8 to 9pm.
The toolkit will be formally launched at Food Matters Live on 20 November. Find out more and register now

by Tanya HAFFNER | Jan 9, 2018 | Thoughts, Media in context, The Nation’s Health, Impactful health initiatives
Each week we analyse some of the hot headlines in health and nutrition news. This week we look at a new ‘Change4Life’ campaign on children’s snacks and the link between processed meats and breast cancer.
HEADLINE 1: LIMIT CHILDREN’S SNACKS TO 100 CALORIES
Popular in the news this week is the new campaign being launched to encourage healthier snacking in children. This has been reported widely, including the BBC, Sky News, The Telegraph, ITV News, the Sun and The Guardian.
Figures have shown that half the sugar consumed by children in England aged 4–10 comes from unhealthy snacks such as biscuits, cakes and sweets, as well and fizzy and juice drinks.
Public Health England (PHE) have launched a new ‘Change4Life’ campaign promoting children’s snacks which are no more than 100 calories. They also advise cutting number of snacks down to twice per day.
The campaign will run for eight weeks and offers money-off vouchers if parents sign up for lower-sugar snacks. Selected supermarkets including Tesco are supporting the campaign.
The Change4Life ‘Food Scanner’ app has also been updated and improved, showing parents the amount of sugar, salt and saturated fat in their food.
Behind the headlines: the Nutrilicious dietetic view
According to the latest National Diet & Nutrition Survey (NDNS), 4–10 year olds consume on average 53.5g free sugars daily – equivalent to 13 teaspoons. Unhealthy snacks and sweet drinks contribute to at least half this daily intake – equivalent to around 7 teaspoons per day.
We discussed the need for free sugars to be limited for children in a previous blog. Improvements must be made in this area and we sincerely hope this campaign can make a difference.
The scale of the problem
According to the new analysis by PHE, every year each 4–10 year old consumes on average 400 biscuits; more than 120 cakes, buns and pastries; around 100 portions of sweets; nearly 70 of both chocolate bars and ice creams; plus over 150 juice drink pouches and cans of fizzy drink.
As these products are predominantly energy dense with few nutrients on offer, looking at the total calorie contribution per year makes the latest findings even more alarming:
| PHE classified unhealthy snacks/drinks |
Energy contribution to children’s diet per year |
| Biscuits |
26,682 kcal |
| Buns, cakes, pastries |
26,682 kcal |
| Sugar confectionery |
5,366 kcal |
| Chocolate confectionery |
10,673 kcal |
| Ice-cream |
10,673 kcal |
| Sweetened soft drinks including sweetened fruit juices |
10,673 kcal |
| Total annual energy intake from unhealthy snacks and drinks |
90,749 kcal |
| Daily calorie equivalent |
249 kcal |
| Weekly calorie equivalent |
1,740 kcal |
The campaign to change habits
A simple ‘rule of thumb’ advice is being promoted by the campaign to help make it easier for busy families to reduce the intake: ‘look for 100 calorie snacks, two a day max’.
While 50kcal saving per day may not seem a lot, over a year that’s a saving of over 18,000 kcals.
It should be noted that the advice does not focus on fruit and vegetables. A variety of these should be encouraged, aiming for a minimum of five portions per day.
Examples of snacks that fall at or below 100 calories include:
- One Soreen malt mini lunchbox loaf (30g) – 95 calories
- One small pot of fruit fromage frais (42-85g) – 45-75 calories
- Snack pack of raisins (14g) – 38 calories
- One banana – 81 calories
- One apple – 51 calories
- One Hartley’s no added sugar jelly pot (115g) – 7 calories
- One packet skinny popcorn (17g) – 57 calories
- One packet Tesco’s lentil curls (20g) – 91 calories
(Source: Values obtained from Dietplan 7 and online supermarkets 2018)
The packaged snacks should also ideally show as greens and ambers on the ‘traffic light’ labelling system (indicating they are not too high in sugar, fat, saturated fat or salt). More information on food labelling is supplied by Change4Life.
It is also useful to check on the label that the portion consumed is what the label portion actually relates to. For example, a large pack of crisps may display the calories for 1/8 of the packet but it can be easy for a child to have more than this portion.
What’s missing from the advice
Although it is positive that action is being taken to promote healthier snacking, the campaign only focuses on the role of calories and may not necessarily teach parents about what makes up a healthy snack.
For example, a handful of nuts would contain more than 100 calories, yet nuts are a nutrient dense food and have many benefits to our health. Snacks can contain less than 100 calories but not contain any valuable nutrients, as in the case of many cereal bars. So, it is questionable how well this campaign will educate parents about healthy eating.
Nevertheless, if improvements can be made to the current eating habits in children it will be beneficial.
HEADLINE 2: EATING BACON, SAUSAGES AND OTHER PROCESSED MEATS INCREASES BREAST CANCER RISK IN OLDER WOMEN
Also in the news this week is the suggestion that eating processed meats will increase the chances of getting breast cancer. This was picked up by the Sun, the Daily Mail, the Evening Standard and the Independent.
The study involved 262,195 women aged 40–69, followed over a period of seven years. For this cohort, a 21% increased breast cancer risk was associated with women consuming more than 9g processed meat per day.
However, when the study was combined with another 10 cohort studies and a meta-analysis performed, the risk was significantly lower.
The meta-analysis found processed meat consumption to be associated with 9% increased risk of breast cancer in post-menopausal women only. No association was found in pre and peri-menopausal women, nor was an association found with red meat consumption.
Behind the headlines: the Nutrilicious dietetic view
The study looked at a variety of processed meats, but clearly the UK headlines are pulling at the Brits’ heart strings by focusing on bacon and sausages.
Firstly, what counts as processed meat? Processed meats are defined as meat which has been preserved through salting, curing, fermentation, smoking or other processes. Examples include sausages, bacon, ham, salami, chorizo, corned beef, hot dogs and pepperoni.
9g processed meat equates to:
- 1 and a bit sausages
- 2½ rashes of back bacon or medium slices ham
- 13 thin 5cm diameter slices of salami
- Almost 3 Peperamis
This study adds further supports to one of the key messages for cancer prevention to avoid processed meat and reduce overall intakes of red meat (no more than 500g per week) whilst focusing on a more plant-based diet.
In order to truly help women reduce their risk of breast cancer, messages like this, focusing on one food type, are not helpful. Study findings should be placed in context of overall dietary and lifestyle advice proven to lower risk as well as regular breast screening checks. This study only found correlation in post-menopausal women and only reported on processed and red meat findings.
With 50,000 new cases of breast cancer every year in the UK, 20,000 of which could be prevented through dietary and lifestyle modifications, there are far more pertinent actions women can take. The World Cancer Research Fund (WCRF) highlights the following as major risk factors for breast cancer:
- Gaining weight in adulthood
- Drinking alcohol
- Being physically inactive
- Not breastfeeding when you have a baby
- Being overweight or obese (for post-menopausal breast cancer)
Although this study further supports the evidence that processed meat isn’t great for women’s health (or, indeed men’s health), we need to stop scare-mongering and instead provide helpful advice to women concerned about the UK’s number one cancer. Scientific findings need to be put into context and then interpreted into practical and helpful advice for consumers.
As well as the lifestyle recommendations by WCRF, it is also important to continue encouraging women to regularly check their breasts for lumps and seek medical assistance if they have any concern as well as attend any breast cancer screening invitation from their health service.
For more tips and advice see World Cancer Research Fund UK and Cancer Research UK

by Tanya HAFFNER | Dec 15, 2017 | Surveys and insights, Changing mindset, Impactful health initiatives, Resources worth having
Currently 2.3 million people in the UK are living with heart disease, at an annual cost of £953m to the NHS. We’re involved in an on-going battle to try to reduce it.
For those in the health industry, the link between high cholesterol and heart disease is well known. Meta-analyses, genetic studies and randomised controlled trials totalling more than 2 million participants, 20 million person-years of follow up and 150,000 cardiovascular events demonstrate a close correlation between cardiovascular disease (CVD) and high levels of low-density lipoprotein cholesterol (LDL-C).
What’s less known is the impact plant stanol esters can have on lowering cholesterol.
Changing behaviours of those at risk of heart disease
GPs and practice nurses are key influencers when it comes to persuading people to change their lifestyle to improve their health. So it’s vital to make sure these healthcare professionals (HCPs) have the facts – and materials – they need to support this.
In a survey we undertook this year of HCPs on behalf of Benecol, we found that persuading patients to improve their diet change is a key priority when it comes to reducing cholesterol – along with cutting smoking and increasing physical exercise.
We discovered that while the HCPs are well aware of the importance of cutting saturated fat and sugar, and want to communicate about healthier eating to patients, they are less likely to know the impact plant stanol esters can have on lowering cholesterol.
Plant stanols and sterols can reduce cholesterol by up to 10% in two to three weeks.
Over 70 clinical studies have demonstrated that plant stanols effectively lower cholesterol.
How do they work?
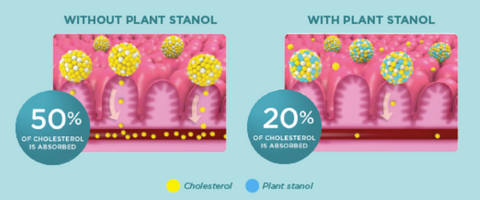
Consumption of foods with added plant stanols or sterols (1.5 – 2.4g/day) should take place at meal times. Mixing with food and digestive juices results in the displacement of dietary and biliary cholesterol in the fat absorption pathways in the gut.

Cholesterol absorption is reduced by about 50% and studies have shown a dose-dependent reduction in circulating LDL-C of 7 – 10% on average.
Cholesterol begins to lower immediately. With continued use full reduction is achieved within 2 – 3 weeks and is sustained over the longer term. What’s more, if used alongside statin therapy, plant stanols lower LDL-C by an additional 10% – an effect greater than doubling the statin dose, which, at best, only provides a 6% additional LDL-C reduction.
Plant stanols provide an easy diet-based solution to all hypercholesterolaemic patients, including those with mildly elevated serum cholesterol level. They would also be especially recommended for those averse to taking statins, anxious to keep statin doses low, or at higher risk from potential statin-related side effects.
They are recommended by a number of prevention and treatment guidelines as part of a cholesterol-lowering diet, including the European Society of Cardiology, the Atherosclerosis Society, UK JBS3 guidelines and the World Health Organisation.
Our holistic communications approach to help reduce cholesterol
As a result of our research, we created a holistic communications approach in association with HEART UK – the Cholesterol Charity and leading heart health dietary specialists – to support practice nurses and GPs, and their patients.
- We created information sheets for the healthcare professionals with full information about dietary changes patients can make to lower LDL-C levels. Included in this was the latest evidence not only on plant stanols but on all dietary recommendations for lowering LDL-C.
- Alongside this were fact sheets for patients, clearly explaining the problem of high cholesterol and the lifestyle changes that would have a significant impact on their health.
We highlighted the key motivators for patients – the fact that a small change would bring quick results.
Companies are accused of only being interested in their profits – and of course, they are ultimately accountable to stakeholders, so money is always going to come into it.
But what we found with Benecol’s approach is that they are genuinely determined to help combat the huge problem of heart disease that exists. Reaching out to health professionals they wanted to understand issues fully and how best to communicate lifestyle change – not just dietary, which would help promote the message of plant stanols, but also more widely, include all dietary matters as well as smoking and exercise.
The materials tell the whole story, educating the professionals and patients and then leaving it in their hands how to act.
Health professionals responsible for communicating heart health cholesterol lowering advice can order these packs by calling the Benecol Helpline 0800 018 4010 and asking for your health professional Benecol Toolkit ‘Small Change, Big Results’ pack.