by Nutrilicious | Mar 3, 2020 | Surveys and insights, Changing mindset
Are you working on a nutrition and health strategy for change? Trying to convince your colleagues or board that your wellbeing approach is right? Developing a new food product and want to know how it will be received from a nutrition, health or sustainability point of view?
Over many years of working with people in the same situation, we know that you’re most likely to succeed if your process includes consulting those who will ultimately be influencing your target consumers – their key influencers including health leaders, NGOs, lobbying groups and health media.
Why carry out qualitative research with influencers?
Too often we’ve seen organisations launch a new initiative without consulting this important audience first – making it far more likely that the initiative won’t be the success it could be.
Do you know who is currently influencing your key target audiences on health and/or sustainability? Do you know what they are saying and might say about you and your initiatives?
These influencers will have a deep understanding of this changing landscape, the sector and the way population groups think and act as well as what they themselves want and may be telling them about your initiative. That’s what makes their insights so valuable – whether you’re using it as proof of an approach and a way to secure funding, or to help shape your thinking.
How to go about getting relevant insights
In 2019, we enjoyed many in-depth, eye-opening conversations with key health and nutrition influencers, carrying out qualitative research for clients. We listened, we learned and we helped companies inform their strategy, sell their vision to their colleagues and boards and develop new products.
The interviewing was vital, and it’s not always easy to get right. Here are our Nutrilicious top things to think about when embarking on your insights-gathering mission:
1. Choose your targets wisely. Work out the ideal criteria for mapping who you want to speak to and why. Always include disrupters and future thinkers if you have a longer term goal.
2. Your interviewee is likely to have a busy day job. Allow sufficient time for chasing appointments and contingency for cancellations.
3. Interviews don’t have to take place in a private space, but make sure it won’t be too loud.
4. Conduct the interview in pairs, to help capture everything but not overwhelm the interviewee.
5. You’re there to listen, not inform. You may be an expert in the field but you need to adopt a beginner’s mindset.
6. Try to extract facts, not opinion, and delve deep. The golden question is ‘why?’. Ask it again and again.
7. If you’re not a qualified practised insights interviewer, it’s important to work with a qualitative researcher or research team to help you. That’s why we partner with See Research. With stakeholder qualitative research we find that a combo team of a nutrition/dietetic expert lead and qualitative researcher is ideal.
8. Always ask permission before recording and don’t video the whole interview, just a summary at the end. You don’t need fancy equipment – a phone on a tripod should be enough, just check that you’re actually recording and your mobile is switched off!
9. If you can’t get a face-to-face meeting, video chat works too, using Zoom, Skype or an equivalent.
10. The interview should just be the beginning of the relationship. Use it as a way to build an understanding of what they care about, which opens doors for future conversations, for you helping them and indeed for them helping you at the communication phase.
11. What will you do with your results? Forget the insights report: it won’t be read widely. Better to paint a picture with infographics and edit your summary videos down to a single short film highlighting the key themes you’ve discovered.
We’re here to help
Hopefully, these points are useful. But if you need more support, we’re here to help – from helping identify your golden targets to delivering the learnings to support your objectives. Just get in contact, we’d love to hear from you.

by Nutrilicious | Aug 19, 2019 | Hot Topics in nutrition, Surveys and insights, Changing mindset
At long last, the Scientific Advisory Committee on Nutrition (SACN) report on saturated fats and health was published this month. The conclusion? Nothing new: saturated fat leads to heart disease and we should limit it to 10% of our calorie intake. So will it finally put an end to the irresponsible advice that abounds suggesting saturated fat isn’t so bad for you?
It’s taken over a year from the draft report to final version because of the number of comments, criticisms and questions as to why certain studies were or weren’t included as part of the overall evidence into sat fats.
The SACN committee has investigated and answered each one, including only the highest quality evidence available. The studies that came to the wrong conclusions about saturated fat were shown to be flawed.
They’re open about certain limitations to the evidence: for example, whether replacing saturated fat intake with carbohydrate can be beneficial. None of the studies look specifically at ‘good’ carbs (for example wholegrain cereals), just at carbs overall. Further research still needs to be done into this.
But the overall conclusion was inescapable: to reduce cardiovascular disease we should lower our intake of saturated fat.
So will high profile influencers like Dr Michael Mosley or Joe Wicks take note and stop promoting ingredients like coconut oil, which is shown to have higher saturated fat than butter and lard?
Sadly, we think it’s unlikely. For one reason or another they seem to have too much invested in it.
But if you’re reading this and feel as strongly as we do about the need to stop the irresponsible advice, join us in canvassing the influencers to open their eyes to the dangers of what they’re suggesting – rather than just thinking about their commercial interests or looking for the next great headline. #saynotosatfat
Go to the British Nutrition Foundation website for a summary of the SACN report findings

by Tanya HAFFNER | Jan 25, 2019 | Hot Topics in nutrition, Surveys and insights
“The world’s diets must change dramatically,” said Harvard University’s Walter Willett, one of the leaders of the comprehensive EAT-Lancet report released this week researching healthy and sustainable diet.
The findings show we must drastically cut down on meat and dairy, and eat more plant foods.
Published after three years of reviewing extensive evidence from around the world, the message is similar to that of both the British Dietetic Association’s One Blue Dot campaign, the government Eatwell Guide, the World Health Organisation and recommendations made by various non-governmental health organisations, for example World Cancer Research Fund (WCRF) and the British Heart Foundation.
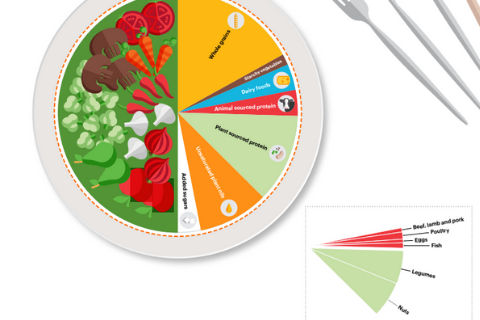
The EAT-Lancet recommended daily diet
Here’s an outline of the recommended daily diet to meet 2,500kcal and all micronutrients:
|
Average recommended intake* |
Comment
|
| Daily |
Weekly |
| Protein foods |
| Beef, lamb and pork |
14g |
98g |
· Less than a quarter pounder per week
· Significantly below the WCRF recommendations of 350-500g per week
· 70-90% below current US & European intakes |
| Chicken and other poultry |
29g |
203g |
· Equivalent to around 1½ chicken breasts per week
· EAT suggests that the poultry allowance can be exchanged for eggs, fish or plant proteins and vice versa |
| Eggs |
13g |
91g |
· Equivalent to around 1½ eggs per week |
| Fish |
28g |
196g |
· Around 1½ – 2 servings a week
· Oil rich fish is strongly recommended as an omega-3 source |
| Legumes: dry lentils, beans, peas & soya foods |
75g |
525g |
· Equivalent to roughly 150g cooked / tinned beans daily
· An allowance within the 75g recommendation for soya products is specified due to the association with lower breast cancer incidence and reduced cholesterol levels |
| Tree nuts & peanuts |
50g |
350g |
· Equivalent to 1½ handfuls daily
· The report acknowledges that some nut and legume crops use intense water farming. However, the evidence for their associated reduced cardiovascular disease, cancer and total mortality risk justified this environmental trade off. |
| Dairy |
| Milk or equivalent in cheese / yogurt etc. |
250g |
1.75L |
· This is a significant reduction in dairy recommendations |
| Carbohydrates |
| Rice, wheat, corn and other, dry weight |
232g |
1.62kg |
· Whole grains advocated
· Equivalent to 1 servings of rice or pasta, 40g serving of breakfast cereals & 2 large slices bread daily |
| Tubers or starchy vegetables |
50g |
350g |
· Equivalent to 1 egg-sized potato daily or 1½ baked potatoes weekly |
| Non-starchy vegetables |
| All vegetables |
300g |
2.1kg |
· Notably, more vegetables than fruit recommended
· 3-4 servings daily |
| All fruits |
200g |
1.4kg |
· 2 servings daily |
| Added fats |
| Unsaturated oils |
40g |
280g |
· Equivalent to 4tbsp oil daily |
| Saturated oils |
≤11.8g |
≤83g |
· An allowance was made taking into consideration using all animal parts
· Equivalent to a single butter pack |
| Added sugars – no more than 5% energy intake – approx. 30g or 7tsp per adult per day. |
* EAT-Lancet recommended diet as well as an average daily intake, also provides a range of intakes.
Some of the notable findings are around red meat for iron and dairy for calcium:
- Iron: There is a problem with deficiency for adolescents but encourages use of inexpensive supplements over consumption of red meat
- Calcium: The United States and other countries over-estimate calcium needs. It is ubiquitous in the diet and there is little evidence that intakes above 500mg per day improve bone health.
The report looks how to change people’s choices to include less meat/dairy, through:
– making healthier foods more accessible and more cost effective
– reducing marketing and availability of unhealthy food.
It also tackles farming changes to a high degree – seen as being as important as, if not more than consumer change.
Conclusion? Change is needed, it’s going to be tough
We need to make big changes in our eating patterns if we’re going to protect our planet and health. It requires a multi-system combined effort approach to reduce food waste/losses, improve food production and encourage dietary shifts.
It is time for everyone to be involved in the urgently-needed transformation of our food system. We’ll be monitoring the impact the report has over time. Stay tuned…

by Tanya HAFFNER | Dec 7, 2018 | The Nation’s Health, Surveys and insights, Education
As Hippocrates, the father of modern medicine, said more than 2,000 years ago, ‘All disease begins in the gut’. And modern science is proving it as true today as it was then.
In this blog we outline the importance of gut microbiota and the use of diet to affect them to try to improve health and welfare.
For a detailed exploration of the topic, register for our free, CPD-accredited NutriWebinar. Led by experts Professor Glenn Gibson and Laura Tilt, it will give you both incredible insight into the science and practical tips on how to help balance gut microbiota for real health benefits.
The importance of the gut microbiome
We have more than 1,000 species of bacteria in our gut. And there’s been an increasing realisation among scientists that these can have a profound effect on our health – from Irritable Bowel Syndrome to infections, asthma and inflammatory disease right through to bone health and cognitive function.
This understanding has led researchers to investigate what we can do to affect the microbiota, to be applied to this wide range of health problems. A steady stream of scientific publications over the last 15 years address the topic, alongside research into probiotics and, more recently, prebiotics – which selectively fertilise the ‘good’ bacteria.
Our gut microbiome status changes throughout our lives. We acquire our gut bacteria mostly at birth. Moving through the milk years, there are differences in acquiring bacteria between breast-fed and infant formulae fed babies: human milk.
There is change again at the weaning stage, after which the gut microbiota remains fairly stable. As we get older there is then a decrease in the largely in beneficial bacteria like the bifidobacteria.
The gut microbiota can be susceptible to various challenges: stress, infection, antibiotics and poor diet all amongst the factor coming into play on a daily basis.
How does diet affect our gut microbiome and our health?
Carbohydrates, proteins, amino acids and lipids are all metabolised by microbiomes in different ways, with different outcomes for our health.
Carbohydrate metabolism – especially that of fibre – leads to organic acids, short chain fatty acids, that have shown to be beneficial in the gut. For example:
- Acetate is metabolised by the muscle, kidney, heart and brain
- Propionate, cleared by the liver, is an appetite regulator also said to be involved in cholesterol synthesis
- Butyrate is a fuel and regulates cell growth
Fibre itself can stimulate the growth of good bacteria. It’s been estimated that per 100g fibre fermented, 30g of bacteria is produced.
Metabolism of excess protein, on the other hand, leads to less positive end products:
- Ammonia induces quick cell turnover
- Phenols/indoles may act as co-carcinogens
- Amines are linked to migraine, cancer, schizophrenia
Balancing our gut microbiota
- Increased fibre intake
To help ensure balanced gut microbiota, our diet needs to include enough fibre. As discussed in our recent blog, government recommendations advise 30g per day for adults, representing a 60% increase in intake for most. Laura Tilt provides excellent advice on how this can be achieved in the NutriWebinar.
- Probiotic and prebiotics
Much work has been done into probiotic supplements: live ‘good’ bacteria that bring health benefits, especially lactobacilli and bifido bacteria.
More recently, scientists have found that prebiotics could have an even more profound effect on our health. They work by selectively proliferating beneficial bacteria, which in turn inhibit pathogens. They may also have a more general effect, including dampening inflammatory issues.
Prebiotics are found naturally in human breast milk and in fructans and inulins in vegetables including asparagus, onion, banana and leeks. They can also be taken as supplements, especially in GOS forms.
Takeaway message
As our understanding of the link between gut microbiota and our health has grown, researchers have increasingly looked to see where we can have the most impact.
We’re in a position where health and nutrition professionals can advise clients on what they can do to improve their gut health and therefore overall wellbeing. We look forward to our research widening and deepening further to improve our understanding in this vital area.
Get involved in the discussion on social media: @Nutrilicious @NutriWebinar #lifelonglearning #feedingthegut

by Tanya HAFFNER | Aug 1, 2018 | Hot Topics in nutrition, The Nation’s Health, Surveys and insights
An extensive detailed analysis of the current scientific evidence into omega-3 seems to have thrown a spanner in the works for heart health dietary advice.
Conducted by Cochrane, the review concludes that there is no correlation between cardiovascular health and intakes of the long chain omega-3 fats eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) over a one- to six-year period.
Long chain omega-3 fats have long been associated with reductions in blood triglycerides, blood pressure and thrombosis; producing anti-inflammatory and anti-arrhythmia effects as well as improving endothelial function and insulin sensitivity.
This most recent publication will raise many eyebrows within the heart health professional arena and likely to be taken up by media editors who seem to enjoy questioning the trustworthiness of public health guidelines. These recommend a diet including omega-3, especially found in oil-rich fish such as salmon, tuna and mackerel.
So, do we need to change dietary guidelines on the importance of omega-3 and oil-rich fish?
Before we jump the gun, it’s important to put things into context:
1. The shortcomings of the review
a. The studies investigated in this review predominantly used omega-3 supplements. Thus the outcomes cannot be related to oil-rich fish consumption which is the main dietary source of EPA and DHA.
b. The studies were also of one to six years’ duration, which is a relatively short period to assess disease and mortality risk. And conclusions cannot be reached for a lifetime consumption of foods rich in EPA or DHA.
c. Many of the studies may not have used adequate number pf subjects in the studies to elicit a result. This is especially the case for studies conducted in healthy individuals (and therefore low risk of heart disease), which would require very high numbers to demonstrate a difference in the omega-3 and non-omega-3 study groups.
d. Any studies conducted over the last two decades of people at risk of cardiovascular disease (CVD) will be in individuals already medicated with statins and other cardio-protective drugs, which may mask the effect, if any, of additional omega-3.
2. Omega-3 benefits go beyond heart health
Long chain omega-3 fats are critical for eye and brain development of the foetus and young children. Therefore, food sources should be included in a healthy balanced diet of children and adults planning for a family.
3. Oil-rich fish is not just omega-3. It offers so many health benefits.
a. Unlike omega-3 supplements, oil-rich fish is a rich source of not only the long chain omega-3 fats but also of selenium, zinc, vitamin D and iodine; woefully lacking in the UK diet.
b. Oil-rich fish has a healthier fat profile when compared to red meat and other animal proteins. Replacing saturated fat with unsaturated fat in the diet has been proven to have a positive effect on blood lipids and cardiovascular health (as confirmed by Cochrane’s 2015 review and the SACN’s & the WHO’s draft 2018 reports). See our saturated fat blog
Indeed, the authors themselves remind us of the other nutritional benefits of oil-rich fish and that this review does not negate public health advice that consuming oil-rich fish is beneficial to health.
The Nutrilicious view
Taking vitamin and mineral supplements as a substitute for eating a healthy balanced diet has never been encouraged by health professionals. However, dietitians recognise that when demands for specific nutrients are high, or when an individual’s nutritional intake is at proven risk of being compromised, supplements can play an important role. For example, pregnancy and folic acid; under-5 year olds and vitamins C and D; or sufferers of osteoporosis and calcium and vitamin D.
Therefore, these findings do not come as any surprise: omega-3 supplements are not a solution to better heart health. There are numerous dietary and lifestyle factors that impact on heart health. It should always be about food rather than the benefits of single nutrients.
As Linda Main, Dietitian and dietary advisor for cholesterol charity HEART UK, explains: “We continue to advise the lifelong consumption of a heart healthy diet centred around eating whole foods rather than the emphasis being on nutrients.
“Eating patterns such as the Mediterranean, DASH or the UCLP© diets result in the consumption of a nutritionally appropriate diet. This is characterised by eating plenty of vegetables, fruits, wholegrains, vegetable proteins such as nuts and soya, seeds, vegetable oils and spreads. In those who consume animal proteins, the inclusion of low fat dairy, lean and largely unprocessed meat and white and oily fish and seafood are recommended.
“Omega-3 supplements are not currently advised by HEART UK and would not be our first choice, except when prescribed by a recognised qualified health professional or when needed to safeguard the intake of the essentially fatty acid – alpha-linolenic acid.”
As oil-rich fish is an excellent low saturated fat protein source, and the main dietary source of long-chain omega-3 fats as well as other crucial nutrients, it should continue to be part of dietary guidelines.
Additionally, for those wishing to follow a more plant-based diet, it’s reassuring that the report finds consumption of the shorter chain omega-3 fats found in plant foods (like rapeseed and soya oil) has cardio-protective qualities. This supports findings from population studies that vegetarians and vegans have a lower incidence of cardiovascular events and mortality compared to non-vegetarians.
Current UK heart health dietary advice remains unchanged:
- Lower the amount of food eaten which is high in saturated fat and replace it with foods high in unsaturated fats (which Cochrane’s 2015 review supports, SACN 2017 Saturated fat draft guidance).
- Increase our intake of fibre (especially from beans, pulses, oats and barley), nuts.
- Consume at least five servings of fruit and vegetables daily.
- Reduce intakes of red meat and avoid/limit processed meat.
- Consume two portions of fish weekly – one of which should be oil rich.
- Increase intakes of leaner and plant-sources of protein.
- Use sterol or stanol fortified products (if blood cholesterol is raised after other dietary changes have been made).
It’s interesting to note that, unlike the US, the UK does not (and has never) recommended taking dietary supplements of omega-3 fish oil.
For up to date expert advice on heart health visit: heartuk.org.uk
Further references
Saturated fat and heart health reports
Supplements for specific groups
NHS UK: Vitamins for children; Vitamins, supplements and nutrition in pregnancy
Vegetarian and vegan diets and health outcomes
- Rizzo N, Jaceldo-Siegl K, Sabate J et al. Nutrient profiles of vegetarian and non-vegetarian dietary patterns. J Acad Nutr Diet.. 2013;113(12):1610-9.
- Sobiecki J, Appleby P, Bradbury K et al. High compliance with dietary recommendations in a cohort of meat eaters, fish eaters, vegetarians, and vegans: results from the European Prospective Investigation into Cancer and Nutrition-Oxford study. Nutr Res.. 2016;36(5):464-77.
- Springmann M, Godfray H, Rayner M et al. Analysis and valuation of the health and climate change cobenefits of dietary change. Proc Natl Acad Sci U S A.. 2016;113(15):4146-51.
- Clarys P, Deliens T, Huybrechts I et al. Comparison of nutritional quality of the vegan, vegetarian, semi-vegetarian, pesco-vegetarian and omnivorous diet. Nutrients.. 2014;6(3):1318-32.
Cochrane is an established body of researchers, health professionals and patients across the globe renowned for their high quality scientific reviews of nutrition and health evidence.

by Tanya HAFFNER | Mar 2, 2018 | Hot Topics in nutrition, Media in context, The Nation’s Health, Surveys and insights, Catering/Out of Home
This week, the Daily Mail and the Independent reported that showing the calorie content of meals in restaurants can help lower people’s calorie intake.
This is based on a systematic review of 28 studies, which concluded that nutritional labelling on restaurant menus can reduce the amount of energy (i.e. calories) purchased.
Overall, it was found that nutritional labelling could reduce calorific intake by up to 12% – around 72 calories for a typical 600kcal meal. That’s equivalent to three boiled new potatoes or around 150ml of juice.
Behind the headlines: the Nutrilicious dietetic view
This study is very relevant, considering that on average we eat out for around a quarter of our meals. These meals can often be served as large portions and can be high in sugar and salt.
More and more restaurants in the UK are now providing the nutritional values of meals, which are often available online. They include Nandos, Starbucks, Prezzo, Wagamama, Zizzis, Giraffe and many more. However, previous research has only shown mixed results as to the effects of having the nutritional values available.
There are some limitations to the review – many of the individual studies it’s based on were graded as poor quality. Nevertheless, it provides evidence that displaying nutritional values to restaurant menus may help to lower calorie intake in individuals.
Another weapon in the battle against obesity
Just this week, Cancer Research UK released a report showing that on current trends 70 per cent of millennials – those born between the early 1980s to mid-1990s – will be overweight or obese by the age 35 to 45.That’s more than any other generation since records began. The UK is already the most overweight nation in Western Europe, with obesity rates rising even faster than in the US. We know definitively from the McKinsey Global Institute Report on Overcoming Obesity: an initial economic analysis that we need as many nudge strategies as possible to help overcome this very serious obesity issue.
Professor Theresa Marteau, the review’s lead author and head of the Behaviour and Health Research Unit at Cambridge University, summed it up: “This evidence suggests that using nutritional labelling could help reduce calorie intake and make a useful impact as part of a wider set of measures aimed at tackling obesity. There is no magic bullet to solve the obesity problem, so while calorie labelling may help, other measures to reduce calorie intake are needed.”
Her thoughts are echoed by many experts. Professor Ian Caterson, president of the World Obesity Federation, stated: “Energy labelling has been shown to be effective – people see it and read it and there is a resulting decrease in calories purchased. Combined with a suite of other interventions, such changes will help slow and eventually turn around the continuing rise in body weight.”
Sue Davies, Which? food policy expert, says it’s not just the experts who believe access to more information is important: “This research highlights the value of calorie information and why it is so important that it is provided more widely for people when eating out. In a recent Which? survey, 63% of people agreed that calorie information should be provided on the food in cafes and restaurants for transparency.”
The United States is leading the way on this front: the Food and Drug Administration recently implemented a policy whereby restaurants with 20 or more locations must show calorie counts on their menus from May 2018. It will be interesting to monitor the impact.
Takeaway message
There are many measures that are needed to help reduce obesity, and the serious health issues that it causes. Ensuring nutritional values are available to consumers may be a simple strategy amongst many that are needed to help individuals take steps to make wiser meal choices.
There are other steps we can take to help us make healthier choices when eating out. The NHS provides some useful advice and tips
At Nutrilicious, we enjoy helping all organisations to implement, measure and communicate nudge strategies to help the nation overcome the urgent problem of obesity. If you would like to discuss how your organisation could contribute, please get in touch – we would be more than happy to discuss and help.